Follow-up
There are many questions you might have about what will happen after your child has surgery. Below are answers to some of the most common questions and concerns.
- How long will my child be in hospital?
- How can I manage the pain following surgery?
- Will my child have a cast?
- How long will the cast be on?
- How can we prevent pressure sores?
- What happens after the casts come off?
- What will it be like at home?
- When can my child stand or walk?
- What is the recovery period?
- What follow-up is needed?
If you have any other questions please discuss them with the Orthopaedic CP team.
The length of time children are required to stay at BC Children’s Hospital following surgery on their legs depends on the type of surgery. Some children can go home the same day while others must say overnight or a few days. Children will usually stay for five to seven days following a SEMLS surgery.
Pain after surgery is normal. During your child’s hospitalization at Children’s Hospital, the Acute Pain Service team will provide expert pain service to manage your child’s pain problems. Their mission is to “STOP PAIN HURTING”. The Acute Pain Service anaesthetist and nurse clinician are experts in managing pain and will see your child daily while in the hospital.
This team will work together with your child’s orthopaedic surgeon and the nursing staff to create and optimize a pain management plan to provide as much comfort with minimum risk or side effects.
The pain-relief medications used are those that are appropriate for the severity of pain your child is experiencing. The Acute Pain Service team will follow your child until your child is comfortable enough to manage with oral medication alone or via a Gastrostomy Tube for those children who receive medications that route.
Resources: What is an epidural infusion?
Managing your child’s pain is important. Since pain from surgery can be very intense in the beginning, your child will be given stronger pain medicines immediately after the surgery. There will then be a step-down to weaker medicine as recovery and pain relief progress.
Your child’s nurse will regularly ask and assess your child’s pain to find out how well the medicine is working. Parents & caregivers are a critical part in helping the health care team to recognize when your child is in pain.
Depending on your child’s age and ability, he/she may be able to tell the nurse how much pain he/she is feeling. The nurses in the hospital will use a pain scale asking your child if he hurts a little or a lot.
If your child cannot speak or does not understand about their pain, there are other ways to check pain. To assess pain, your child’s nurse will also watch your child for signs such as crying, moaning, fussing, frowning, playing or sleeping. Watch your child carefully and see what you think. Parents often know if their child has pain or is uncomfortable in any way. It is very important for parents to let their child’s nurse know what their child’s behaviour is like when they are in pain and any other comfort measures that help.
Speak to your child’s nurse if you think your child is in pain!
What is a spasm? It is an uncontrolled, usually fast, muscle jerk that might or might not be visible to others. Spasms are often related to increased pain your child is experiencing.
Muscle spasms can be common after your child’s orthopedic surgery. When muscles are cut or stretched during the surgery, they can react by going into spasm. It is important to know that your child may also receive a medication to help control muscle spasms.
If your child has been taking medicines to manage his/her muscle spasms already before having surgery, the amount (dosage) of the medicine might be increased for a period of time post operatively and when they go home from the hospital.
Some things you should know about your child’s post-operative pain:
- Children do not all feel pain the same way
- Your child will likely have pain after his/her surgery.
- In the days after the surgery, the pain should get better, not worse
- Pain medicines will help your child hurt less. Always follow the directions given to you by the nurse, doctor, nurse practitioner or pharmacist.
- Comforting your child will help him/her relax & relieve pain.
- Distracting your child can also help relieve pain.
- Comfort & distractions can be as important as giving medicine to your child.
- Check how much pain your child has 1 hour after you give pain medicine.
Before you leave the hospital, your child’s nurse, surgeon, doctor or nurse practitioner will tell you how you can help your child when he/she hurts. You may be given a prescription for pain-relief medications and be advised about giving medicines that are available without a prescription for pain relief.
The day he/she goes home, if your child is in pain, you can give him/her some pain relief medicine regularly during the rest of the day, and the next few days too, if needed.
You will help your child to hurt less, by giving pain-relief medicine regularly in the first few days after your child is home.
- Follow the directions of the prescription medication bottle and the non-prescription pain-relief medication bottle/package.
- Pain after surgery is normal.
- Do not wait to give pain relief medicine until your child is in a lot of pain.
- For many children it is good to give pain-relief medicine in the morning to get their day started and at bedtime to help with sleep.
- Taking pain relief medicine regularly (even at night) is important.
- Prevention of pain is better than treatment. It is important to give pain medicines regularly.
- Pain relief medicine works better if your child takes the medicine before the pain gets strong.
- After the first few days, when your child hurts less, give the medicine only when he needs it. You will know when he/she says it hurts. The way he/she acts may also show you that your child is in pain. Some pain-relief medicines can cause stomach upset. Avoid giving these medicines on an empty stomach.
- Parents can help make the best pain relief decisions for their own child because they know their children best.
Note: If your child was given medicine to manage “muscle spasms”, continue to give the medicine as prescribed by the Orthopedic Surgeon/Doctor.
If your child is still in pain or muscle spasms are getting worse or if you have questions/concerns:
Please call your Doctor, Orthopaedic Surgeon’s office or the Orthopedic Nurse Clinician for advice.
You can expect ups and downs with pain relief. It is common to have times when your child’s pain increases – especially when their activity, home exercise program and physiotherapy increases.
Some children have discomfort when their casts are removed in the weeks following surgery. It is important to give your child some pain-relief medicine before this procedure.
Some children experience anxiety or pain when their position is moved or during any range of motion/home exercise/physiotherapy sessions, especially the first time their legs are moved.
Consider giving your child pain-relief medicine 30 minutes to 1 hour before a therapy/exercise session is planned to improve comfort.
Maybe! There are many types of casts and splints. The type your child has will depend on which surgical procedures are done. Please discuss your child’s plan with the orthopedic CP Team.
Most children who have lower leg or foot surgery will have this type of cast. It starts below the knee and covers the foot.
Long leg casts are used most often with surgeries around the knee. These casts go from the top half of the thigh to the ankle with the knee straight. Your child will not be able to bend their knees.
Changes to wheelchairs will be made so that your child can sit with their legs out straight. If your child uses ankle foot orthotics (AFOs), the occupational therapist may mould resting foot splints that fit over top of the cast to keep your child’s feet in a good position.
Zimmer splints are similar to long leg casts but they are made of material and have Velcro straps to keep them in place. After the surgery, changes to the wheelchair will be made so that your child can sit with their legs out straight.
An abduction pillow can be used with soft tissue procedures such as adductor lengthening. The pillow is a foam wedge that’s sits in-between your child’s legs to keep them wide apart. It may also be used after a VDRO once the cast has been removed.
This splint is sometimes used after a VDRO or adductor release. It is custom made for your child by the orthopaedic occupational therapist. It starts up at the groin and goes all the way to the ankles. There is a bar that holds the legs wide apart.
After the surgery, changes to the wheelchair will be made so that your child can sit in their chair while wearing the splint. If your child uses ankle foot orthotics (AFOs), the occupational therapist may mould resting foot splints that fit over top of the cast to keep your child’s feet in a good position.
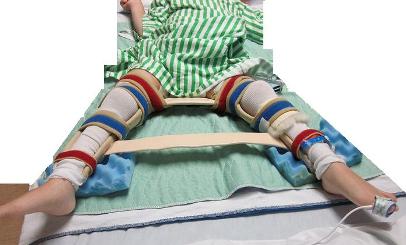
Abduction (Petrie) splint
Most children who have a VDRO and adductor muscle lengthening will have this type of cast. It starts up at the groin and goes all the way to the ankles. The legs are positioned out straight and are spread wide apart. They are kept apart by putting a wooden bar between the two casted legs.
After the surgery, changes to the wheelchair will be made so that the child can sit in their chair while wearing the cast. If your child does not have a wheelchair or adaptations are not possible, a different chair will be loaned to you.
If your child uses ankle foot orthotics (AFOs), the occupational therapist may mould resting foot splints that fit over top of the cast to keep your child’s feet in a good position.
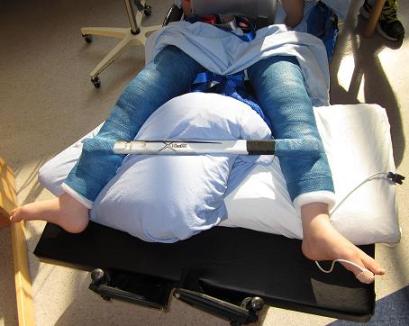
Abduction (Petrie) cast
The length of time in the cast will depend on the type of surgery and the amount of healing seen on x-ray. Casts may be on anywhere between 3 and 8 weeks . Please discuss your child’s specific plan with the orthopedic CP team.
While your child is in a cast or splint it is very important to watch their skin. Children in casts and splints are at risk for pressure sores.
For detailed information about what a pressure sore is, why and where they happen, and how to prevent them please read the The Added Pressure of Surgery: Preventing Pressure Sores After Your Child’s Surgery.
Your child will be able to move more and sometimes this will hurt. This is not unusual and should decrease within a few weeks. In order to help minimize discomfort you should bring some pain medication to the clinic on the day the cast is being removed.
Do not force any movements when moving your child. Even though the cast has been removed, the bones are not fully healed.
Positioning is important as the bones and muscles continue to heal. If your child was in a Abduction (Petrie) cast the occupational therapist may make an Abduction (Petrie) splint or give you an abduction pillow. The splint/pillow may be required all the time for a few more weeks or just at night time.
Children can typically return to their usual wheelchair seating. If the child had hip surgery or adductor lengthening it is recommended that the wheelchair has a pommel or another method of keeping the legs separated.
Your child’s physiotherapist and occupational therapist on the hospital unit will review what your child can and cannot do after surgery. They will show you how to move your child in the cast and teach you how to position your child so they are comfortable. The nursing staff will review how to perform personal care while your child is in the cast and how to care for the cast.
Continue with pain medicine as prescribed by the doctor before you leave the hospital.
Change your child’s position frequently (every 2 hours). Use pillows or blankets to help with comfort. Pillows and blankets should also be used under boney or prominent areas to prevent pressure on the skin. During position changes and transfers caregivers should use proper techniques to protect their own bodies. Have your child help as much as they can and are allowed.
Check the skin daily for any signs of pressure areas. Call the clinic with any concerns.
Encourage and help your child to get out of bed and into their wheelchair throughout the day. As much as possible, resume your normal routine and activities.
Arrange a visit from your community physiotherapist and occupational therapist. They may be able to help with mobility in the home, adaptations, equipment, positioning, activity ideas, etc.
Physiotherapy is essential after surgery. The Orthopaedic CP team will discuss when it is appropriate to begin therapy.
Please check with the orthopedic CP team about any restrictions for your child. If your child had surgery on their bones, they will not be allowed to stand or put any weight on their legs for several weeks. When your child can begin to stand will depend on how quickly their bones heal. This is different for each child. Your child will usually be allowed to begin putting some weight on their legs at 6 weeks. The pool is a great place to gradually begin weight bearing.
If your child had soft tissue surgeries only there may not be any weight bearing restrictions. The orthopedic CP team will review this with you.
Each child has different abilities and, therefore, recovery will also differ for each child. After a SEMLS or complex surgery, we expect it will take children at least 6-12 months to return to the same level of function as before the surgery. It may take up to a year to regain full strength and mobility. Physiotherapy is important during this time period.
You will have a follow up appointment a few weeks after surgery. At this appointment you will have your child’s incisions checked and you may have an X-ray. This is an excellent opportunity to discuss any questions you may have (i.e. concerns about pain medication, constipation, etc…).
Your child will need continued monitoring after the surgery. As your child grows, there can be risk that the problem will occur again. Therefore, it is very important that you return to the Orthopedic Clinic for follow up visits.
If your child had plates or screws placed in their hips these may be taken out 1 year after their first surgery. This will be done during another surgery. Your child will stay in the hospital for 1-2 nights and they may not be able to stand or put weight through their legs for 2 weeks. There is no casting or splinting required when plates and screws are removed.
